Could the mere power of optimistic thought be sufficient to enhance one’s immune system? A recent investigation suggests that this may indeed be the case, offering novel perspectives on the synergistic integration of psychological and physiological health strategies.
This concept is not as implausible as it may initially appear. Scientific inquiry has established a profound connection between our cognitive processes and our physical well-being, with the placebo effect serving as a prime example that strong conviction in a therapeutic intervention can precipitate tangible physiological advantages.
Within the framework of a novel randomized controlled trial, an academic contingent from Tel Aviv University in Israel discovered that individuals who successfully amplified activity in a brain region associated with reward exhibited a more robust antibody response following administration of a standard vaccine.
“These observations indicate that intentionally cultivated positive anticipation can leverage reward circuitry to modulate immune function—a mechanism that could potentially be employed for non-invasive immune enhancement,” state the authors in their peer-reviewed publication.
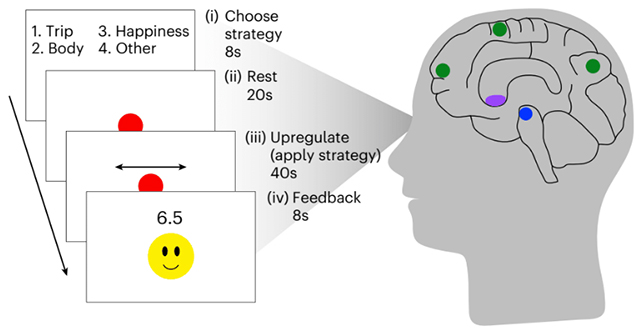
A total of eighty-five subjects were allocated into three distinct experimental cohorts.
One cohort utilized a neurofeedback apparatus that guided them through cognitive exercises aimed at augmenting neural engagement within the brain’s mesolimbic pathway, commonly referred to as the reward circuit.
Functional Magnetic Resonance Imaging (fMRI) neurofeedback empowers individuals to visualize their own neural activity, thereby facilitating the acquisition and refinement of mental strategies designed to stimulate specific brain areas. For the inaugural group in this research endeavor, successful enhancement of mesolimbic pathway activity resulted in a progressively more felicitous facial expression appearing on a digital display.
A secondary cohort participated in analogous neurofeedback instruction, demanding a comparable degree of cognitive exertion but concentrating on cerebral regions not intrinsically linked to reward processing. The third group received no neurofeedback intervention.
Following the completion of 3 to 4 training modules by the neurofeedback cohorts, all attendees were inoculated with a hepatitis B virus (HBV) vaccine, a standard agent employed in studies investigating immune responses. Levels of HBV-specific antibodies were subsequently quantified at intervals of 14 and 28 days post-vaccination.
Individuals who successfully executed tasks designed to activate a specific component of the mesolimbic pathway, namely the ventral tegmental area (VTA), demonstrated the generation of a significantly greater quantity of HBV-specific antibodies, indicative of a heightened immune response—although the vaccine’s actual efficacy was not a primary measurement point.
Significantly, VTA activation correlated with augmented production of HBV-specific antibodies when participants were anticipating a pleasurable event, such as an upcoming vacation, thus suggesting the involvement of the placebo phenomenon.
“Given the absence of evidence supporting alternative explanations, our findings propose a top-down cerebral-immune regulatory mechanism, analogous to that previously elucidated in rodent models,” the researchers articulate.
While comparable outcomes have been observed in animal subjects, this study offers compelling empirical evidence that volitional positive cognition can exert influence over immune function in humans, although extensive further exploration is warranted.
“Despite presenting a potential neurological intervention for augmenting vaccine-induced immune responses in humans, the participant sample size in our investigation is considered comparatively modest,” the authors concede.
The ramifications of these discoveries suggest that therapeutic strategies aimed at fostering positive expectations could serve as a valuable adjunct to conventional medical treatments. Such interventions might be designed to target neurochemical signals that support immune function, including dopamine.
The research team proposes that their methodology “may be utilized to explore novel avenues for fortifying immune processes, with potential implications for disciplines such as cancer immunotherapy and the management of chronic inflammation.”
“Consequently, it may be possible to leverage the inherent capacities of our minds and brains to facilitate bodily recuperation during periods of exigency,” the researchers conclude.