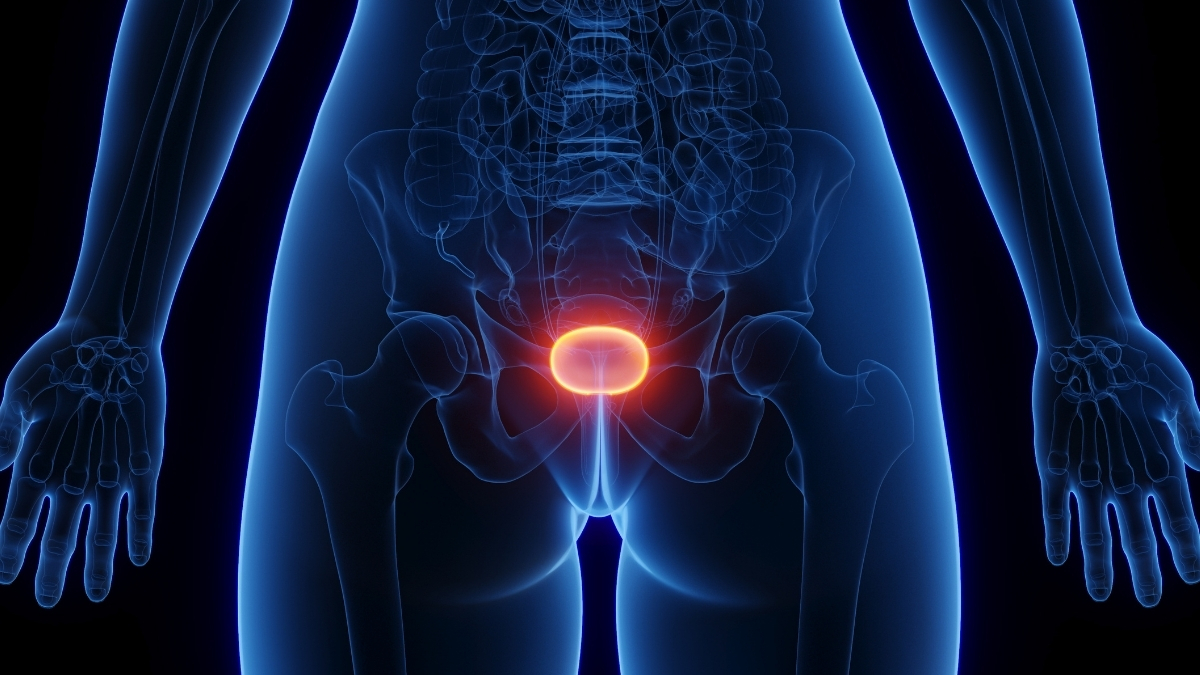
Urology services across England and Wales are observing a discernible upturn in the caseload of individuals aged 16 to 24 presenting with cystitis, a condition frequently linked to ketamine consumption.
This phenomenon appears to run parallel to an escalation in ketamine usage. Data indicates a significant increase in the number of adults and adolescents seeking treatment for ketamine dependency in the past year, a marked jump from figures reported just a few years prior.
The abuse of ketamine can precipitate a spectrum of adverse effects on the bladder, manifesting as urinary frequency, nocturia, sudden and urgent needs to urinate, urinary leakage, inflammation, discomfort in the bladder or lower back, and hematuria.
These symptoms can attain a severe intensity, profoundly disrupting daily functioning and, in certain unfortunate instances, may result in irreversible damage.
Ketamine was initially authorized for human medical application in 1970, serving as an anesthetic. More recently, scientific investigations have posited that ketamine, when administered in reduced dosages, might exert mood-elevating properties.
However, a burgeoning cohort of individuals is now engaging with ketamine for recreational purposes.
Its pharmacological action classifies it as a dissociative agent, inducing sensations of detachment from one’s physical self and immediate environment. It is capable of eliciting hallucinogenic, stimulant, and analgesic effects, which typically persist for one to two hours.
Users commonly inhale powdered ketamine nasally or smoke it, administer liquid ketamine via injection, or incorporate it into beverages to experience its psychoactive effects. Nasal insufflation usually yields more potent effects and more conspicuous symptoms compared to oral ingestion.
Individuals who use ketamine can rapidly develop a tolerance to its effects, necessitating augmented dosages to achieve the same subjective experience. This phenomenon is likely attributable to the body and central nervous system’s adaptive mechanisms that enhance the efficiency of drug metabolism.
Those who engage in frequent ketamine use often find themselves requiring double the quantity compared to sporadic users to elicit comparable effects.
Urinary Tract Compromise
Persistent, high-dosage ketamine consumption can inflict severe damage upon the bladder, the entire urinary conduit, and the renal system. In extreme prognoses, the bladder may necessitate extirpation.
The pioneering documented instances of ketamine adversely impacting the bladder surfaced in Canada in 2007, where nine individuals with a pattern of recreational ketamine use exhibited profound bladder pathology and hematuria. Subsequently, an extensive investigation conducted in Hong Kong identified analogous pathological findings in 59 individuals who had utilized ketamine for an extended duration exceeding three months.
Ketamine, in common with all xenobiotics, undergoes metabolic transformation within the organism, culminating in its breakdown and subsequent elimination via the renal system.
During its metabolic degradation, ketamine is converted into chemical compounds that possess the potential to inflict substantial injury upon the bladder lining. When these resultant metabolites remain in prolonged apposition with the tissues of the urinary tract, they exert an irritant effect and compromise tissue integrity.
The bladder typically sustains the initial insult, owing to its physiological function of urine retention. Subsequently, the ureters, which serve as conduits between the kidneys and the bladder, as well as the kidneys themselves, can also become implicated.
With the passage of time, the bladder may undergo shrinkage and develop rigidity, giving rise to pronounced voiding symptoms. The ureters can become stenotic and exhibit angulation, a presentation sometimes characterized as resembling a “walking stick.” This pathological alteration can precipitate urine stasis within the renal pelvis, a condition known as hydronephrosis.
Furthermore, ketamine amplifies oxidative stress, a process that leads to cellular damage and consequent apoptotic demise of bladder epithelial cells. This cascade of events compromises the protective urothelial barrier, rendering it permeable and hyper-responsive.
The cumulative impact of these pathological alterations can result in an overactive, exquisitely sensitive, and painful bladder, frequently precipitating intense micturition urges and episodes of urinary incontinence.
The pathological progression of ketamine-induced bladder injury unfolds in distinct phases.
During the initial phase, the bladder becomes inflamed. This inflammatory state is often amenable to reversal through cessation of ketamine use and targeted pharmacotherapy, which may encompass anti-inflammatory agents, analgesics, or prescription medications designed to mitigate urinary urgency and facilitate urothelial healing.
In the subsequent phase, the bladder may exhibit contracture or develop fibrotic rigidity. Treatment at this juncture mirrors that of the initial phase, with the potential addition of intravesical irrigation. This procedure involves the instillation of therapeutic agents directly into the bladder via a catheter. The administered medication serves to coat the bladder’s luminal surface, aiding in the restoration of its protective functions and ameliorating inflammation.
Intramuscular injections of botulinum toxin may also be employed to induce detrusor relaxation, thereby alleviating bladder spasms and associated pain and urgency. Sustained abstinence from ketamine remains paramount to arresting further pathological progression.
The terminal phase is characterized by irreversible damage to both the bladder and renal parenchyma. Over time, if renal involvement becomes significant, it may culminate in chronic kidney disease and eventual renal failure. Hemodialysis, a life-sustaining intervention that rectifies fluid and electrolyte imbalances and removes uremic toxins from the bloodstream, or even surgical reconstructive procedures may be necessitated to restore renal function and the integrity of the urinary apparatus.
Despite its classification as a Class B controlled substance since 2014, ketamine unfortunately remains remarkably affordable and readily accessible, with street prices in certain UK locales as low as approximately £3 per gram. Elevating public awareness regarding the perilous consequences of ketamine consumption is therefore indispensable in the prevention of these grave health sequelae.
![]()