Portal hypertension (PH), a significant sequela of liver cirrhosis, is characterized by a pressure differential exceeding 5 mmHg between the portal vein and the inferior vena cava. When the hepatic venous pressure gradient (HVPG) surpasses 10 mmHg, the condition attains clinical significance, with a marked escalation in complications, thus rendering prompt identification imperative for therapeutic guidance.
A recent scholarly examination, disseminated online on March 1, 2025, and formally published on March 17, 2025, within the esteemed journal Portal Hypertension & Cirrhosis, investigates the potential of advancements in sonographic technology to furnish a dependable, non-invasive modality for the assessment of PH.
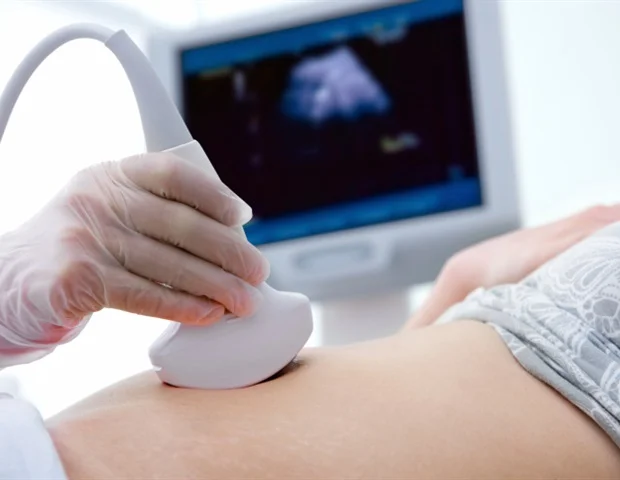
PH emerges when hepatic blood flow encounters augmented resistance, predominantly attributed to cirrhosis, precipitating an elevation in portal venous system pressure. The review meticulously details the capacity of various ultrasound methodologies to delineate these physiological alterations.
Conventional B-mode ultrasonography is adept at revealing the structural hallmarks of cirrhosis, such as a tessellated hepatic surface, aberrant liver morphology, and enlarged vascular structures, in addition to indirect indicators of PH, including splenomegaly and ascites.
Doppler ultrasonography empowers clinicians to meticulously evaluate the directionality and velocity of blood flow within the portal vein and contiguous vasculature. In cirrhotic states, portal venous flow frequently decelerates, and in advanced presentations, it may even reverse its trajectory, a phenomenon designated as hepatofugal flow, signifying profound PH.
Given that no solitary metric comprehensively encapsulates disease severity, practitioners judiciously integrate multiple sonographic parameters, a methodology referred to as multiparametric ultrasound.
Elastography, another technique elucidated in the review, quantifies hepatic tissue stiffness, serving as a proxy for the progression of fibrosis and the magnitude of PH.
The research personnel also highlight contrast-enhanced ultrasonography, which characterizes hepatic hemodynamics through the meticulous tracking of an administered contrast agent traversing hepatic vasculature. Nevertheless, individual variations in flow dynamics and the development of compensatory collateral vessels can introduce complexities to interpretation.
While ultrasonography has not yet supplanted invasive pressure measurements entirely, multiparametric ultrasound presents a pragmatic, non-invasive alternative that can assist clinicians in achieving a more profound understanding of the intricate transformations inherent in hepatic pathology, thereby bolstering both patient surveillance and clinical decision-making.
Notably, the investigation also proffers scenario-specific sonographic recommendations, thereby augmenting its practical utility for both medical practitioners and research scholars.
Möller, K., et al. (2025). Portal Hypertension – Noninvasive Multiparametric Ultrasound‐Based Criteria and Measurements. Portal Hypertension & Cirrhosis. DOI: 10.1002/poh2.70002. https://onlinelibrary.wiley.com/doi/10.1002/poh2.70002