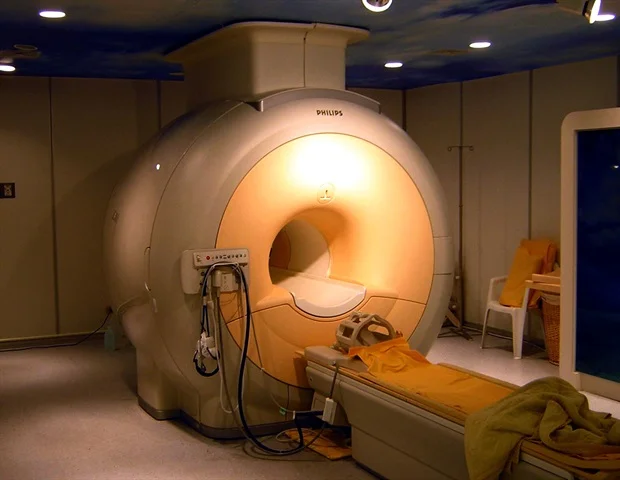
A novel approach utilizing magnetic resonance imaging has been devised by investigators associated with the Biomedical Data Science Laboratory (BDSLab) at the ITACA Institute of the Universitat Politècnica de València. This innovative technique facilitates the objective measurement of the progression of highly aggressive brain malignancies, with a particular emphasis on glioblastoma.
This research undertaking, which has been documented in the esteemed scientific publication Medical Physics, confronts a significant impediment in the diagnosis and therapeutic management of this specific tumor type: its pronounced propensity to infiltrate adjacent healthy brain parenchyma.
Within the scope of their investigation, the BDSLab contingent from the UPV has introduced a pioneering biomarker, designated as the Dynamic Infiltration Rate (DIR). This metric possesses the capability to delineate distinct patterns of neoplastic proliferation and to independently forecast patient prognoses.
Historically, diagnostic and assessment methodologies have predominantly relied on monitoring the augmentation of tumor dimensions or the displacement of cerebral structures. These approaches have fallen short in adequately capturing the nuanced mechanisms of tumor growth or its biomechanical ramifications on the surrounding neural tissue.”
Carles López Mateu, lead author of the study
The foundational research was executed by Carles López Mateu, María Gómez Mahiques, F. Javier Gil Terrón, Víctor Montosa i Micó, Juan M. García-Gómez, and Elies Fuster García. Their efforts were further bolstered by collaborative partnerships with researchers hailing from Oslo University Hospital.
Cerebral Biomechanics
The sophisticated biomarker developed by the UPV’s BDSLab-ITACA collective integrates the volumetric expansion of the tumor over a temporal continuum with the mechanical forces that this expansion exerts upon contiguous brain tissue. Through a longitudinal analysis of magnetic resonance imaging data, the research team has successfully generated detailed tissue compression maps. These maps provide critical insights into the extent to which the tumor compresses or invades healthy neural tissue.
The DIR biomarker serves to synthesize these two critical phenomena, thereby enabling a distinction to be made between tumors that exhibit hyper-proliferative tendencies accompanied by substantial brain compression and those that are more characterized by infiltrative growth without significant compressive effects.
“This index affords us the ability to characterize the tumor’s biological behavior in a manner that transcends its mere physical dimensions, furnishing vital intelligence regarding its inherent aggressiveness,” articulated Carles López.
The efficacy of this methodology has been rigorously substantiated through the utilization of both simulated datasets and two international clinical cohorts comprising glioblastoma patients. The empirical findings unequivocally demonstrate that the DIR facilitates a robust stratification of patients based on their predicted outcomes.
“Individuals exhibiting low DIR values demonstrate an average survival period of 35.2 weeks. In stark contrast, those with elevated DIR values have an average survival of merely 16.0 weeks,” emphasized María Gómez Mahiques, a researcher at ITACA and a contributing co-author of the study.
Collectively, these findings underscore the significant potential of the DIR as a valuable adjunct in clinical decision-making processes, empowering clinicians with a more precise characterization of tumor aggressiveness.
Advancing Personalized Medical Interventions
The collaborative research endeavors undertaken by the UPV team and their counterparts at Oslo University Hospital are instrumental in propelling the field towards more individualized medical care. This is achieved by facilitating the tailoring of therapeutic interventions and follow-up regimens to align with the specific growth trajectory of each individual tumor.
“This constitutes a quantitative, consistently reproducible, and non-invasive biomarker, exclusively derived from medical imaging. It serves to amplify the critical role of biomedical engineering and data science within the domain of precision oncology, while simultaneously leveraging accessible methodologies that are conducive to its future integration into clinical practice,” the authors concluded in their summation.
López‐Mateu, C., et al. (2026). Biomechanical mapping of tumor growth: A novel method to quantify glioma infiltration and mass effect. Medical Physics. DOI: 10.1002/mp.70334. https://aapm.onlinelibrary.wiley.com/doi/10.1002/mp.70334