The United States has not seen the approval of a new male contraceptive method since the 1980s.
However, by 2026, a range of alternatives to traditional condoms and vasectomies are anticipated to become available.
The subsequent generation of male contraceptives is currently undergoing phase 2 human clinical evaluations. In parallel, following extensive research in murine models, scientists at Cornell University have successfully identified a method to impede sperm genesis within the testes at a crucial developmental juncture.
The experimental contraceptive drug demonstrated efficacy, safety, and reversibility in male mice. Within six weeks following the cessation of injections, normal sperm production was re-established, and two subsequent generations of offspring were born without any observable abnormalities.
“Our research group is virtually unique in advocating for the testis as a feasible target for contraceptive intervention to halt sperm production,” states geneticist Paula Cohen from the Cornell Reproductive Sciences Center.
The research team’s focus is on a fundamental biological process known as meiosis, which is integral to mammalian testicular function.
Meiosis follows mitosis, a process where stem cells differentiate into sperm precursors. Meiosis involves a cell containing two full sets of chromosomes dividing to produce four new cells, each possessing half the chromosomal complement necessary for life, which then mature into spermatozoa.
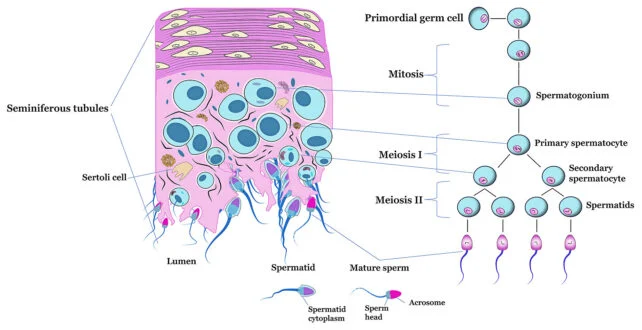
“Meiosis presents a natural regulatory point in spermatogenesis, where temporary inhibition could facilitate precise and reversible control over fertility,” contend Cohen and her collaborators.
The critical aspect is to avoid eradicating self-sustaining stem cells prior to mitosis, as this could precipitate irreversible sterility. However, once these stem cells proliferate and undergo differentiation, there exists a potential for them to egress from the testes as mature sperm, thereby enabling fertilization.
The compound designated JQ1 intervenes at an opportune moment. Initially formulated to inhibit the proliferation of cancerous tumors, it has now demonstrated efficacy in preventing sperm stem cells from engaging in meiosis.
Further comprehensive safety evaluations are requisite before human trials can commence. Nevertheless, Cohen and her associates propose that their investigation furnishes a “framework for the development of novel contraceptive strategies that operate safely and with selectivity within the germline.”
Currently, male contraception options are limited to vasectomies and condoms. However, recent retrospective analyses indicate that male respondents express a willingness to explore new contraceptive modalities if such choices are made available.
A significant concern revolves around the potential for adverse or undesirable side effects associated with contraceptive interventions. Analogous to female contraception, the likelihood of such occurrences can be elevated with hormonal approaches.
“A primary motivator for our research was to identify nonhormonal contraceptive targets within the testis, aiming for a method that curtails sperm production without impacting male sexual drive or secondary sexual characteristics,” elucidates Cohen, referencing attributes such as facial and chest hair development or vocal deepening that emerge during puberty.
“Our findings indicate a substantial recovery of normal meiosis and complete sperm functionality, and crucially, that the resulting offspring exhibit no developmental anomalies,” Cohen affirms.
While this represents encouraging progress, there remains a developmental pathway to traverse before JQ1 can be subjected to human testing. A male contraceptive agent, YCT-529, which targets sperm precursors before the meiotic stage, entered phase 2 clinical trials last year and may achieve market availability sooner.
“The progression of reversible male contraceptives toward clinical application has been notably limited,” the authors observe.
“The realization of reversible, nonhormonal male contraceptives continues to be a critical unmet requirement for the attainment of reproductive equity.”
This study’s findings were published in the Proceedings of the National Academy of Sciences.