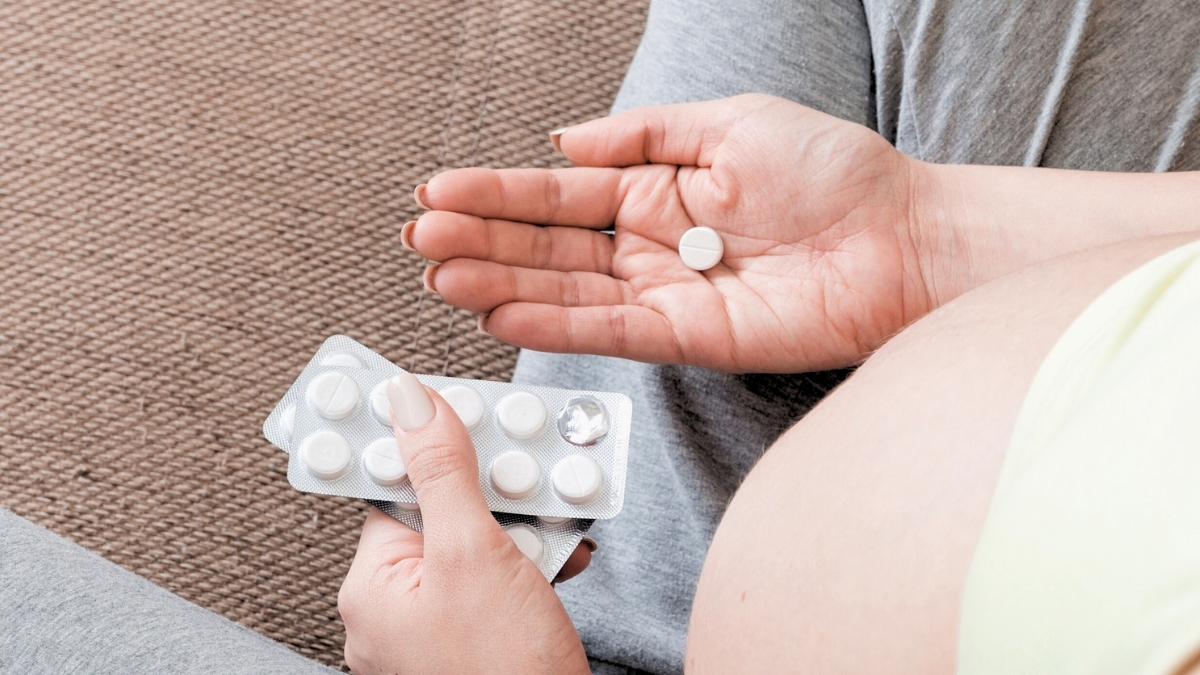
Individuals who have experienced pregnancy in recent months might have encountered a specific quandary. The onset of symptoms such as a fever, intense headache, or discomfort in the back can prompt a moment of reflection. The question arises: is it permissible to administer paracetamol?
Such hesitation is understandable. In September of the preceding year, governmental authorities in the United States introduced considerable uncertainty and apprehension by suggesting a correlation between paracetamol consumption during pregnancy and the development of autism and attention-deficit hyperactivity disorder (ADHD).
However, a significant new global investigation, unveiled concurrently in the esteemed journal The Lancet, offers a much-needed resolution.
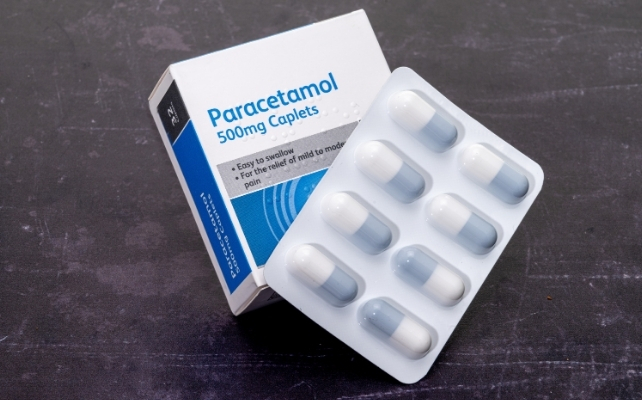
This research substantiates that the ingestion of paracetamol – also recognized as acetaminophen, or by commercial designations like Panadol and Tylenol – does not elevate an infant’s susceptibility to autism, ADHD, or cognitive impairment when utilized during gestation.
Paracetamol continues to be a secure and effective agent for alleviating fever and pain throughout any phase of pregnancy.
Key Findings of the Recent Investigation
The investigative team conducted a comprehensive systematic review and meta-analysis. This methodology involved aggregating findings from numerous prior studies rather than focusing solely on a single cohort.
Collectively, they scrutinized 43 distinct investigations examining the potential for an increased incidence of autism, ADHD, or intellectual disability in children exposed to paracetamol in utero.
Critically, the researchers prioritized sibling-comparison studies. These studies involve comparing siblings within the same family, where paracetamol use during pregnancy differed between them.
This analytical framework yields superior comparative data, enabling researchers to isolate the specific variable under investigation – namely, paracetamol exposure.
The shared genetic makeup, domestic setting, and familial background of siblings minimize potential confounding variables that could otherwise skew the research outcomes.
Sophisticated statistical techniques were employed by the authors to ensure the precision and reliability of their conclusions.
The Research Outcomes
Upon analysis of these higher-caliber studies, the research team identified no statistically significant escalation in the risk of autism, ADHD, or intellectual disability among children whose mothers had utilized paracetamol during pregnancy.
This observation remained consistent across various analytical strata, including (a) analyses confined to sibling studies, (b) examinations focusing on studies exhibiting minimal risk of bias, and (c) evaluations of children monitored for over five years.
In essence, when employing the most robust methodologies, the previously reported alarming associations were demonstrably unsubstantiated. The study concludes that paracetamol, when administered as directed, continues to be safe throughout pregnancy.
These findings are in alignment with those of another seminal study conducted in 2024. The Swedish research encompassed nearly 2.5 million children born between 1995 and 2019.
The Swedish investigation underscored the imperative of rigorous controls in scientific inquiry.
It revealed that studies lacking sibling comparison as a means to mitigate confounding factors appeared to indicate a marginal increase in the risk of autism and ADHD associated with paracetamol use during pregnancy.
However, when researchers applied stringent statistical methodologies in sibling studies to account for inherent individual differences, such as genetics or living conditions, these apparent associations were nullified.
The Swedish study, mirroring the current Lancet publication, also found no empirical evidence to support an elevated risk of autism, ADHD, or neurodevelopmental disorders with paracetamol use during pregnancy.
Significance of These Findings
Paracetamol is not merely an over-the-counter medication; it frequently represents the sole recommended therapeutic option for managing pain and fever in pregnant individuals.
The Therapeutic Goods Administration, the Australian regulatory body for medication safety and quality, reaffirms paracetamol’s status as a pregnancy “Category A” drug. This classification signifies its safety for use during pregnancy when taken as prescribed.

The ability to rely on a safe medication to reduce fever is of paramount importance for expectant mothers.
Failing to address fever during pregnancy can pose detrimental effects to both the developing fetus and the mother. Elevated body temperature during gestation has been associated with adverse outcomes including miscarriage, premature birth, and complications during delivery.
Consequently, abstaining from paracetamol “just in case” is not a prudent safeguard. The potential risks of untreated pain or fever may outweigh those associated with the medication itself.
For individuals who are pregnant and contemplating the use of a tablet for nighttime fever or pregnancy-related discomfort, this study should provide reassurance regarding the safety and evidence-based nature of paracetamol use.
Paracetamol continues to hold its position as the primary therapeutic choice, a role it has fulfilled for many years.
Should any concerns arise, consultation with a healthcare provider is strongly recommended.
![]()