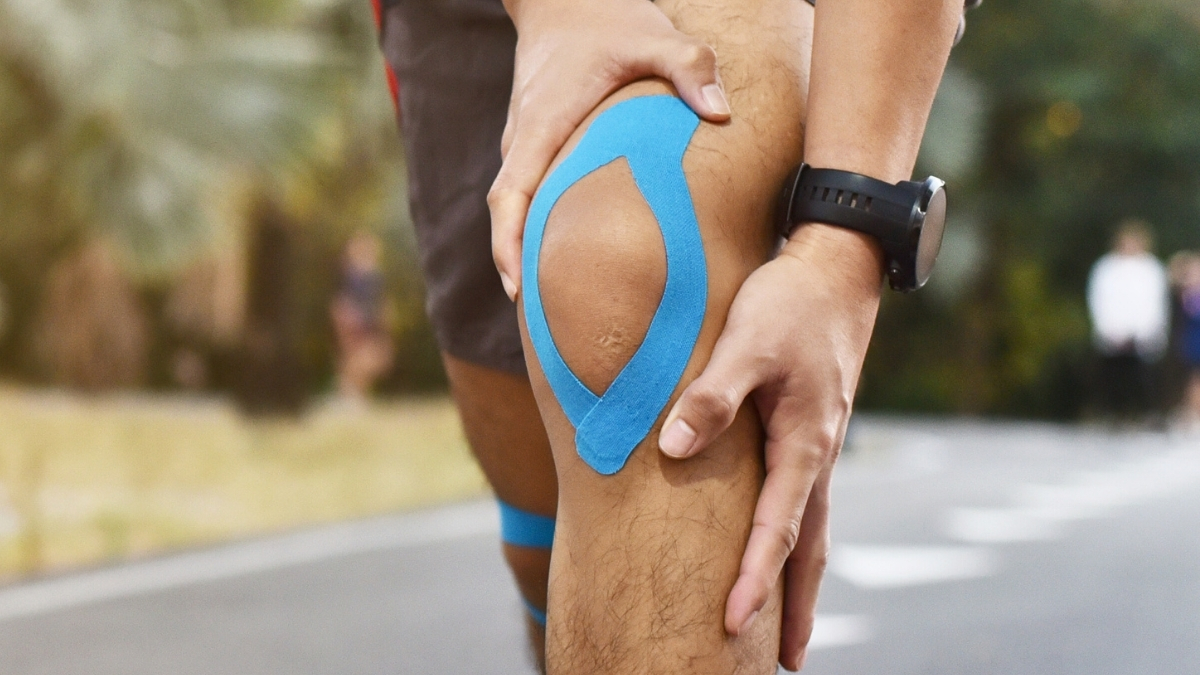
Osteoarthritis is a prevalent degenerative joint condition characterized by discomfort, rigidity, and effusion, leading to diminished joint mobility. While frequently impacting the knees, hips, and hands, it can manifest in other bodily articulations.
For individuals diagnosed with osteoarthritis, engaging in physical activity is a commonly recommended intervention by healthcare professionals. This approach has become a cornerstone of contemporary therapeutic guidance in recent times.
Nevertheless, a recent meta-analysis indicates that the efficacy of exercise may not be as substantial as initially presumed.
However, a more granular examination of this research reveals certain caveats, suggesting that it should not be interpreted as a rationale for discontinuing one’s exercise regimen.
Methodology of the Review
The research cadre undertook an “umbrella review” – a comprehensive synthesis of existing systematic reviews. This methodology involves aggregating and scrutinizing data from individual studies to address a particular inquiry. By examining previously published systematic reviews, a broader perspective on a given research subject is achieved.
Following an extensive search of numerous studies, the researchers incorporated five principal systematic reviews, encompassing 100 distinct studies and involving 8,631 participants. Additionally, they integrated the findings from 28 more recent clinical trials, which included an additional 4,360 individuals.
Utilizing this amassed dataset, the study evaluated the impact of exercise on knee, hip, and hand osteoarthritis. This was juxtaposed against various comparative interventions, such as inactivity, sham treatments, educational programs, manual therapies, analgesic medications, injections, and surgical procedures.
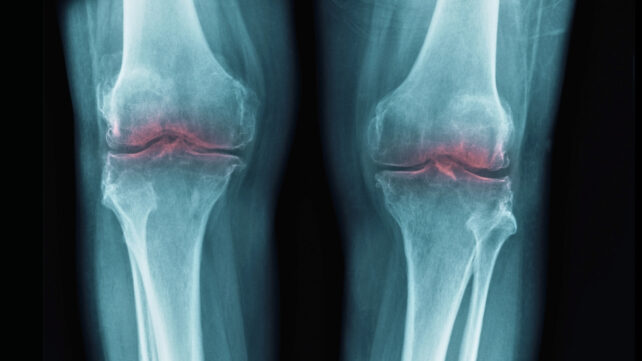
Findings of the Investigation
When contrasted with inactivity and placebo interventions, exercise was associated with modest improvements in pain reduction for the hip, knee, and hand, registering between 6 and 12 points on a 100-point scale.
Conversely, exercise did not demonstrate a superior enhancement in functional capacity compared to either of these control groups.
For osteoarthritis affecting the knee and hip, evidence suggested that exercise yielded comparable pain reduction and functional improvement to pharmacological interventions like ibuprofen and intra-articular corticosteroid injections aimed at mitigating inflammation. These pharmaceutical approaches also achieved pain alleviation in the vicinity of 5–10%.
The investigators concluded that exercise was less efficacious in augmenting pain relief and functional outcomes than a complete joint replacement procedure for patients with knee and hip osteoarthritis.
Identified Limitations of the Study
Firstly, the authors aggregated all forms of exercise into a single category. This meant that resistance training, cardiovascular exercise, flexibility exercises, hydrotherapy, and Tai Chi were all treated identically.
This is a significant oversight, given that the effectiveness of different exercise modalities varies. Prior systematic reviews have indicated, for instance, that aerobic exercise might be optimal for alleviating pain and enhancing function in individuals with knee osteoarthritis, whereas stretching exercises were found to be least effective.
Furthermore, the researchers did not differentiate based on the participants’ clinical severity. Existing research suggests that individuals experiencing more severe pain and poorer function at the commencement of an intervention tend to exhibit more pronounced responses to exercise compared to those with milder symptoms and better baseline function.
Secondly, the review did not distinguish between supervised and self-directed exercise programs.
However, studies have demonstrated that supervised training leads to significantly superior outcomes compared to unsupervised training, likely due to the presence of a trainer who provides guidance and encouragement.
Thirdly, the authors failed to account for the duration of the exercise interventions. The majority of the study periods were relatively brief, averaging around 12 weeks.
It is plausible that adherence to an exercise regimen over an extended period would yield more favorable results, thereby allowing for a greater scope of improvement than that achievable through short-term engagements.
Consequently, the findings of this review may not accurately represent the benefits attainable from exercise for individuals with osteoarthritis who are committed to consistent physical activity as a sustained component of their weekly health regimen (which is frequently advised).
Finally, the review did not consider the prescribed dosage of exercise. Improvements in pain and function appear to be dosage-dependent, increasing with the total weekly exercise volume in individuals with osteoarthritis. One meta-analysis, for example, revealed that optimal benefits were observed at approximately 150 minutes of moderate-intensity exercise per week.
These identified limitations suggest a potential underestimation of exercise’s benefits for osteoarthritis by this recent review.
Enhanced Well-being: Physical and Mental
Notwithstanding the limitations of the review, the minor pain reductions reported could still substantially enhance an individual’s quality of life. A 10% decrease in pain can translate into a meaningful improvement in mobility, capacity for work, social engagement, and the ability to provide care for others.
The review also indicated that exercise can achieve comparable pain reduction to non-steroidal anti-inflammatory drugs and corticosteroids, without the associated adverse effects or financial outlay.
Furthermore, physical activity can positively influence cardiovascular health, elevate mood, assist in weight management, and mitigate the risk of developing chronic conditions such as cancer and diabetes.
These multifaceted benefits can profoundly impact an individual’s overall health and happiness.
Recommendations for Action
Based on the disclosures within this recent review, individuals can feel assured that any form of physical exertion is likely to yield some degree of pain relief.
However, drawing upon prior scientific evidence, it is probable that more substantial and comprehensive health advantages can be realized through sustained engagement in exercise.
The most effective exercise is one that is consistently performed. For those who find pleasure in outdoor activities and walking, this represents an excellent choice, as it will contribute to improvements across all health dimensions and alleviate pain.
Moreover, if pain levels permit, individuals should not hesitate to occasionally increase the intensity of their workouts to a point where engaging in conversation becomes somewhat challenging.
For individuals who prefer a gym environment, strength training is also associated with significant general health benefits, particularly when integrated as a long-term practice.
![]()