Emerging research on sleep patterns and the timing of nightly rest delivers a salient message for individuals aiming to mitigate their susceptibility to significant cardiovascular ailments, such as myocardial infarctions or cerebrovascular accidents: adherence to a consistent bedtime is paramount.
While prevailing health investigations frequently concentrate on the caliber and extent of slumber, this recent inquiry, conducted by academics at the University of Oulu in Finland, has illuminated that the regularity of retiring for the night can be a crucial determinant, particularly when sleep duration does not exceed eight hours.
The investigative team meticulously quantified sleep behavior metrics for a cohort of 3,231 subjects at the age of 46. Sleep activity was assiduously monitored utilizing wearable technology over a seven-day period.
Upon categorizing participants who logged less than eight hours of sleep into distinct groups—consistent, somewhat consistent, and inconsistent—based on their nocturnal habits, the resultant data revealed that individuals in the inconsistent category exhibited a twofold elevation in their predisposition to a severe cardiac episode within the subsequent decade, in comparison to their counterparts who maintained a regular schedule.
Furthermore, a greater degree of fluctuation in the sleep ‘midpoint’—the temporal point midway between commencing sleep and awakening—was also correlated with diminished cardiovascular well-being.
“Our discoveries imply that the constancy of bedtime, specifically, may hold considerable importance for cardiac health,” states medical researcher Laura Nauha.
“It serves as a proxy for the oscillations inherent in daily life and the extent to which these rhythms are disrupted.”
An important qualification, however, is that this observed risk association was exclusively discernible among individuals who reported less than an average nightly sleep duration, just shy of eight hours. It appears that obtaining sufficient restorative sleep acts as a protective buffer against the hazards associated with an erratic bedtime.
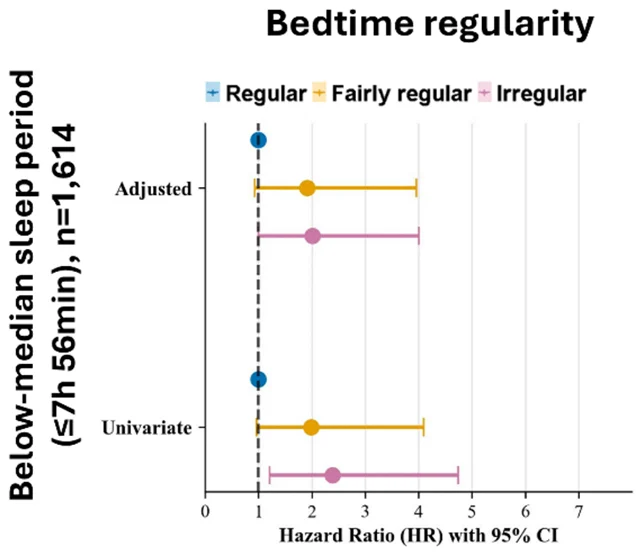
Notably, the data indicated that variations in wake-up times did not appear to exert a similar influence. The discernible correlation was confined to substantial discrepancies in the timing of sleep onset. Within the inconsistent group, the average variability in bedtime throughout the week amounted to 108 minutes, contrasting sharply with the 33 minutes observed in the regular group.
Although the researchers meticulously accounted for confounding variables such as blood pressure, sex, and physical activity levels, it is imperative to acknowledge that causality cannot be definitively established from this investigation; only a significant association has been identified.
The scientific team posits that the intrinsic 24-hour biological cycles governing our physiology—our circadian rhythms—may offer a potential explanation for a portion of this observed link. Disparate bedtimes on successive nights are likely to perturb and disrupt these endogenous rhythms, consequently impairing the heart’s capacity to undergo adequate restorative processes.
The contemporary study also concedes that the impact of real-world stressors could be a considerable contributing factor. Daily life challenges that impinge upon sleep schedules—such as occupational demands or mental health concerns—frequently exert a parallel adverse effect on cardiovascular health.
“Prior investigations have drawn connections between irregular sleep patterns and cardiovascular risks; however, this represents the inaugural instance we have differentiated between the variability of bedtime, wake-up time, and the sleep midpoint, examining their independent associations with major cardiac occurrences,” advises Nauha.
For the purposes of this particular study, major cardiovascular events were formally defined as conditions necessitating specialized medical intervention, encompassing myocardial infarctions (commonly known as heart attacks) and strokes.
It is also pertinent to contextualize these findings. Out of the more than 3,000 participants involved, 128 experienced such an event during the ten-year observational period, indicating a relatively low incidence rate overall.
Moreover, sleep was exclusively monitored for a seven-day duration, and it is plausible that participants’ established routines may not have remained consistent throughout the entirety of the study period.
Notwithstanding these considerations, cardiovascular diseases continue to represent the predominant cause of mortality on a global scale, accounting for approximately 18 million fatalities annually based on the most recent available data. This clearly underscores the urgent need for effective interventions in managing this critical health concern.
The research group expresses a strong desire for subsequent investigations to delve into this bedtime-cardiovascular relationship with greater granularity, and across broader, more heterogeneous populations, not least because bedtime is a behavioral element over which many individuals possess a degree of personal agency.
A burgeoning body of evidence consistently links both the quality and regularity of sleep to a wide spectrum of health outcomes. Furthermore, it is well-established that many of these interdependencies—such as the interplay between sleep and physical activity—operate in a bidirectional manner. The insights derived from this study provide an additional actionable target for enhancing our overall sleep-related health.
“Sustaining a consistent sleep schedule stands as one modifiable factor that a majority of us can influence,” observes Nauha.
The findings of this research have been formally published in the esteemed journal BMC Cardiovascular Disorders.