Schizophrenia is identified as a severe psychiatric ailment characterized by psychosis, which impairs an individual’s capacity to distinguish reality from delusion.
This condition affects approximately one percent of the Canadian populace and is associated with significant health complications, including a reduction in life expectancy.
A confluence of elements can elevate the susceptibility to developing schizophrenia. These encompass prenatal environmental influences (such as nutritional deficiencies or exposure to substances), a familial predisposition, childhood adversities, and residing in urban settings during formative years.
Nevertheless, definitive biomarkers for predicting early-stage risk remain elusive. This deficiency is particularly impactful, given that timely diagnosis significantly enhances treatment efficacy and patient prognoses.
Current research endeavors are investigating the placenta as a potential reservoir for early indicators of schizophrenia susceptibility.
The Placenta-Brain Nexus
The placenta serves as a narrative repository of gestational events, capable of reflecting both optimal and compromised fetal conditions. This concept, termed the placenta-brain axis, posits that adverse placental impacts can detrimentally affect fetal brain development, with consequences extending into both the immediate and distant future.
Extensive clinical investigations have revealed alterations in specific genetic signatures within the placentae of pregnancies yielding infants with low birth weight. These placental markers demonstrate a robust correlation with an elevated predisposition to schizophrenia and other adverse neurodevelopmental outcomes (encompassing conditions like autism and cognitive deficits) in offspring.
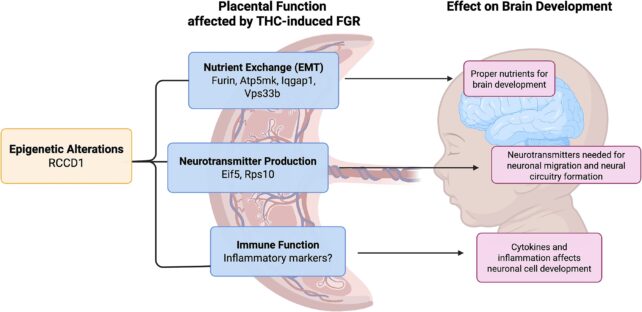
Furthermore, substantial evidence links maternal cannabis consumption during gestation to detrimental impacts on fetal brain development, including an amplified risk of schizophrenia.
This is a matter of particular concern in Canada, where cannabis was legalized in 2018. Since that time, prenatal cannabis use has seen an upward trend, with the most frequently reported incidence being 24 percent among expectant adolescents (aged 13 to 19 years).
While the association between prenatal cannabis exposure and low birth weight is established, the extent to which cannabis exposure influences the same placental biomarkers linked to schizophrenia remains inadequately understood.
My research laboratory, possessing prior experience in examining the effects of prenatal drug exposure, addressed this inquiry in a study recently published in Biology of Reproduction in January.
THC Exposure Investigation
In my capacity as a professor within the Department of Obstetrics and Gynaecology at Western University’s Schulich School of Medicine and Dentistry, I collaborated with my research cohort and esteemed colleagues, including Master of Science candidate Andrea Kocsis, Dr. Enzo Perez Valenzuela, Dr. David Natale, and Dr. Steven Laviolette. Our collective objective was to ascertain whether THC, the primary psychoactive constituent of cannabis, induces alterations in these recognized placental markers associated with schizophrenia.
Initially, we employed a preclinical rodent model where expectant female animals were administered edible THC incorporated into Nutella. Our observations indicated that both male and female progeny exposed to THC exhibited diminished prepulse inhibition during their early developmental stages. Prepulse inhibition serves as a psychometric assessment tool frequently utilized in the diagnostic evaluation of schizophrenia in human subjects.
Specifically, the prepulse inhibition paradigm quantifies sensorimotor gating – the brain’s capacity to attenuate extraneous sensory information – by monitoring the dampening effect of a subtle, antecedent stimulus (the prepulse) on the startle response elicited by a subsequent auditory pulse.
Crucially, our findings revealed that the placentae of offspring exposed to THC displayed elevated levels of several human placental markers previously identified as being linked to schizophrenia risk.
Subsequently, we investigated the replication of these effects in a human cellular culture model. Our experiments demonstrated that isolated human placental cells subjected to short-term (24-hour) treatment with THC exhibited comparable increases in the expression of these schizophrenia-associated genes.
Risk Identification and Mitigation
This research carries significant clinical ramifications. While cessation of cannabis use during pregnancy remains the unequivocal recommendation, practical challenges, including social dependence or habitual patterns, can make this difficult for many individuals. Consequently, some infants are exposed to cannabis prenatally without any agency.
By identifying cannabis-specific placental markers associated with schizophrenia, there exists a prospective avenue for mitigating adverse developmental trajectories early in life through psychotherapeutic or nutritional interventions.
Considering that schizophrenia typically manifests between the ages of 16 and 30, the ability to identify risk at birth would represent an invaluable diagnostic advance. Moreover, placental assessment post-delivery could emerge as a pragmatic method for evaluating schizophrenia risk.
Further investigative research is warranted to elucidate whether other cannabis constituents, such as cannabidiol (CBD), exert comparable influences on neurodevelopment or modify these placental markers.
It is likewise imperative to explore the predictive capacity of these markers for other adverse outcomes, including psychiatric disorders, autism spectrum disorder, or cognitive impairments.
Furthermore, given that the pre-conception health and lifestyle choices of both paternal and maternal figures can impact placental development, it is plausible that cannabinoid consumption by either parent prior to conception could compromise placental integrity and escalate schizophrenia risk, though this hypothesis necessitates additional empirical scrutiny.
In the interim, our findings furnish critical functional insights for healthcare practitioners and regulatory bodies, such as Health Canada, as they continue to formulate policies and guidelines pertaining to the safety of cannabis consumption during pregnancy.






