A novel metric, which scrutinizes underlying biological indicators of metabolic well-being rather than merely height and mass, is now offering refined estimations of disease susceptibility. This new approach goes beyond conventional measurements.
A recent investigation, spearheaded by scientific personnel at the University of Gothenburg in Sweden, indicates that an elevated metabolic Body Mass Index (MetBMI) correlates with an increased likelihood of developing type 2 diabetes and associated ailments.
The conventional Body Mass Index (BMI), a straightforward calculation of weight divided by height, has recently faced re-evaluation regarding its efficacy as a health barometer. While simple to compute, it overlooks critical aspects such as the specific anatomical distribution of adipose tissue and the efficiency with which the body converts ingested nutrients into usable energy.
This research team posits that MetBMI could furnish a more precise evaluation. Their comprehensive analysis unveiled a molecular fingerprint indicative of metabolic impairment, discernible in the byproducts generated by gut microorganisms during the digestive process.
“Our MetBMI metric illuminates a latent metabolic derangement that may not always be apparent from the numbers on a scale,” states endocrinologist Rima Chakaroun, affiliated with the University of Gothenburg. Her insights highlight the limitations of conventional weight-based assessments.
“Individuals with identical BMI values can exhibit vastly different risk profiles, contingent upon the functional efficacy of their metabolic processes and adipose tissue behavior.”
The investigators leveraged health data and biological samples from 1,408 participants to construct an algorithm designed to ascertain MetBMI. This algorithm focused on specific blood metabolites that serve as indicators of biological process functionality.
“Circulating metabolites, intricately influenced by an individual’s genetic makeup, dietary habits, and the composition of their gut microbiome, provide a comprehensive, system-level assessment of metabolic health that extends beyond the simple measurement of excess body weight,” the researchers elaborate in their published work.
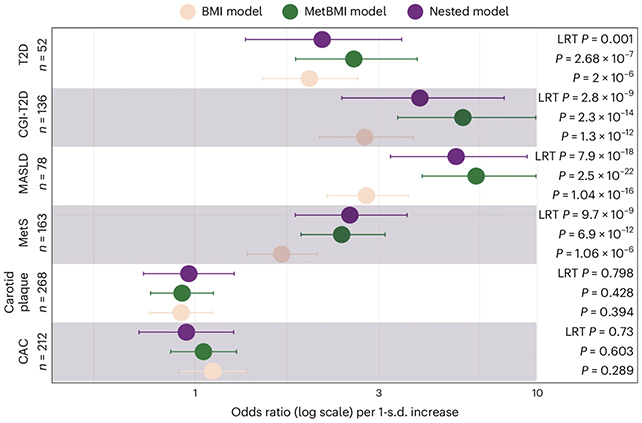
Subsequently, this MetBMI algorithm underwent rigorous testing on an independent cohort of 466 individuals. It proved to be a reliable predictor of both body fat quantity and its distribution. Furthermore, it significantly outperformed standard BMI in forecasting the presence of diabetes, fatty liver disease, and other metabolic disorders.
Participants exhibiting a MetBMI that was disproportionately high relative to their body mass faced a 2.6-fold increased likelihood of having type 2 diabetes and up to a five-fold heightened risk of metabolic syndrome, a condition frequently recognized as a precursor to diabetes.
The implications of this research extended further: the study also uncovered a robust association between MetBMI and the gut microbiome. Elevated MetBMI scores were linked to a less varied bacterial ecosystem and a diminished presence of microorganisms capable of metabolizing dietary fiber.
“The specific metabolites that significantly inform the MetBMI assessment are, in fact, either modified by or produced by the gut microbiota, effectively functioning as a type of metabolic regulator,” explains Fredrik Bäckhed, a biomedical researcher at the University of Gothenburg. This perspective underscores the gut’s pivotal role.
This observation suggests that interventions targeting gut bacteria, such as dietary adjustments and physical activity regimens, could potentially enhance metabolic health indicators that are not readily apparent through conventional weight measurements.
In a subsequent analysis involving 75 individuals who underwent bariatric surgery, those with higher MetBMI scores demonstrated less post-operative weight reduction. This finding further reinforces the notion that metabolic health plays a crucial role in effective weight management.
While MetBMI necessitates additional validation prior to widespread clinical adoption, these preliminary findings suggest its potential to become a more precise and dependable prognostic tool for obesity-related diseases, surpassing the predictive capabilities of mere weight measurements.
“Traditional BMI frequently fails to identify individuals who, despite maintaining a normal weight, possess a substantial metabolic risk,” comments Bäckhed. He emphasizes the need for a more nuanced approach.
“MetBMI has the capacity to facilitate a more equitable and accurate evaluation of disease risk, thereby paving the way for more individualized strategies in prevention and treatment.”