Researchers at Stanford University, alongside their collaborators, have engineered a novel artificial intelligence model capable of forecasting an individual’s susceptibility to over 100 medical conditions, even while they are in a state of slumber.
As elucidated in a recently published academic article, the SleepFM AI system scrutinizes a comprehensive array of physiological data captured during sleep to anticipate an individual’s future risk of developing dementia, experiencing heart failure, and overall mortality – based on a solitary night’s rest.
SleepFM operates as a foundation model, akin to ChatGPT, having been trained on an extensive repository of nearly 600,000 hours of sleep data sourced from 65,000 participants. While ChatGPT derives insights from textual content, SleepFM acquires knowledge from 5-second segments of sleep data extracted from recordings originating from various sleep diagnostic centers.
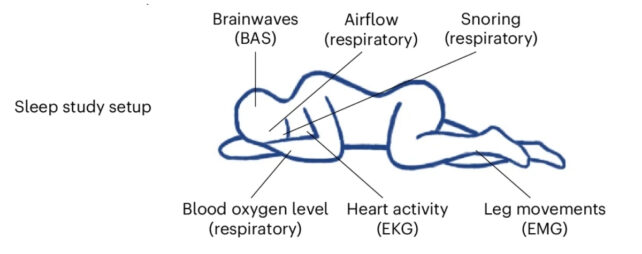
These datasets were meticulously collected by sleep specialists utilizing a rigorous, albeit potentially uncomfortable, methodology known as polysomnography (PSG). This technique, regarded as the benchmark for sleep analysis, employs a multitude of sensors to monitor neurological activity, cardiac function, respiratory patterns, and limb and ocular movements during unconsciousness.
“During our investigation of sleep, we gather an impressive volume of signals,” remarked Emmanuel Mignot, a Stanford professor of sleep medicine and a co-senior author of the paper.
The investigative team validated SleepFM’s capabilities through a newly devised learning paradigm termed leave-one-out contrastive learning. This approach involves systematically omitting data from one specific modality, such as pulse measurements or airflow patterns, thereby compelling SleepFM to infer the absent information by synthesizing it from other available biological data streams.
To incorporate a critical component for predictive accuracy, the researchers subsequently correlated the PSG data with tens of thousands of long-term health outcome reports from patients spanning a wide demographic spectrum, encompassing health records extending up to 25 years of post-sleep study follow-up.
Following an exhaustive analysis of over 1,041 distinct disease categories identified within the health records, SleepFM demonstrated the capacity to predict 130 of these conditions with a notable degree of precision, solely based on a patient’s sleep data.
The AI exhibited particular proficiency in forecasting the likelihood of cancers, pregnancy-related complications, cardiovascular ailments, and psychiatric disorders, “achieving a C-index exceeding 0.8.”
“A C-index of 0.8 signifies that in 80 percent of instances, the model’s prognostication aligns accurately with the actual health trajectory,” stated James Zou, a biomedical data scientist at Stanford and another co-senior author of the publication.
SleepFM also performed commendably according to the AUROC classification framework, which assesses its competence in differentiating between individuals who will and will not experience a particular health event within a defined 6-year prediction window.
In comparative evaluations, SleepFM surpassed existing predictive models, demonstrating exceptional accuracy in forecasting Parkinson’s disease, myocardial infarction, cerebrovascular accidents, chronic renal disease, prostate and breast cancers, and all-cause mortality. These findings further underscore the well-established correlation between suboptimal sleep patterns and adverse health sequelae, potentially serving as an early indicator of underlying conditions contributing to poor sleep.
While certain data types and sleep phases proved to be more insightful predictors than others, the highest predictive power was derived from observing the intricate interdependencies and discrepancies among various physiological functions.
Specifically, the most robust disease indicators emerged from physiological processes that appeared incongruous: “a brain exhibiting signs of sleep while the heart appears alert, for instance, seemed to portend adverse outcomes,” clarified Mignot.
The research team acknowledges certain limitations, including the evolution of clinical methodologies and variations in patient demographics over recent decades. Furthermore, the dataset predominantly comprises individuals referred for sleep studies, implying that a segment of the general population may be underrepresented in the PSG data.
Notwithstanding the controversies surrounding AI in domains such as artistic creation, its profound implications for healthcare serve as a compelling testament to the indispensable and scientifically remarkable capabilities of artificial intelligence systems. For instance, future applications might integrate SleepFM with wearable sleep-tracking devices to enable continuous health monitoring.
Thus, just as large language models (LLMs) adeptly decipher human discourse by analyzing linguistic relationships, “SleepFM is fundamentally learning the language of sleep,” posited Zou.
This groundbreaking research is disseminated in Nature Medicine.






