An episode of migraine is considerably more severe than a common headache.
Migraine is a debilitating neurological disorder characterized by intense head pain, often accompanied by nausea, vomiting, and heightened sensitivity to light and sound.
Approximately five million Australians are affected by migraine, yet the distinct phases of an attack are not widely understood.
Familiarity with the four distinct stages can empower individuals to recognize the signs and implement effective pain management strategies at each juncture.
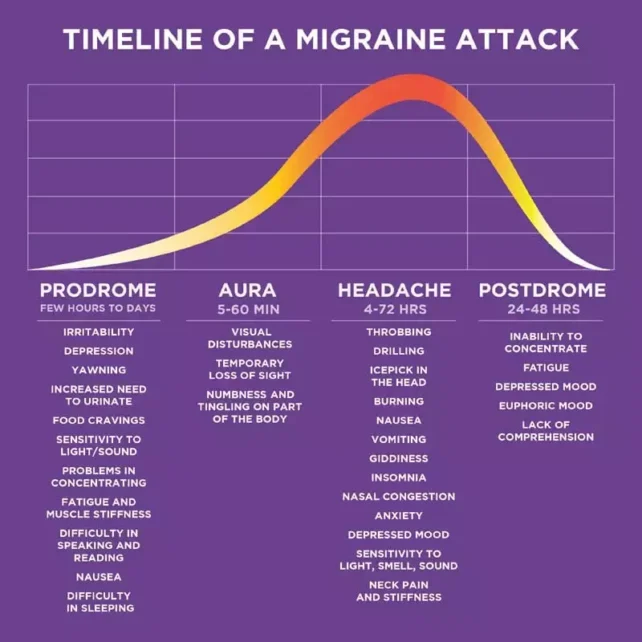
Stage 1: Prodrome
The initial manifestation of a migraine is referred to as the “prodrome” or “premonitory” phase. This serves as an early warning period, commencing approximately 24 to 48 hours prior to the full onset of a migraine episode.
The prodromal phase is significantly influenced by the hypothalamus, a critical brain region responsible for regulating fundamental physiological processes such as body temperature, appetite, emotional state, and sleep patterns.
During a migraine event, the hypothalamus exhibits abnormal activation. Given its intricate connections to other brain areas with diverse functions, this aberrant activity can consequently disrupt their normal operation.
This disruption may manifest as symptoms like impaired concentration, intense food cravings, heightened irritability, and insomnia. Identifying these early indicators can significantly increase the likelihood of intercepting the onset of a migraine and initiating timely treatment.
Stage 2: Aura
The second phase of a migraine attack is termed “aura.” Aura encompasses a range of transient neurological phenomena that can affect vision, speech, or sensory perception. Visual auras, primarily impacting sight, are the most prevalent form.
Symptoms associated with visual aura might include the perception of flashing lights, shimmering patterns, or the appearance of blind spots. Sensory auras can present as numbness or tingling sensations in the face or extremities. In more severe instances, individuals may encounter difficulties with articulation.
Current research points to a process known as cortical spreading depression as a contributing factor to aura symptoms. This phenomenon involves a slow-moving wave of electrical activity that propagates across the cerebral cortex, potentially affecting the function of specific brain regions.
It is noteworthy that only about 30% of individuals experiencing migraines also report the presence of aura.
Stage 3: Headache
The third phase is characterized by the headache itself. This is when individuals typically experience a throbbing or pulsating pain, often accompanied by symptoms such as nausea and increased sensitivity to light and sound.
Without intervention, this phase usually persists for a duration of four to 72 hours.
The activation of various neural networks during a migraine episode can lead to the emergence of additional symptoms beyond the headache.
When the medulla, often referred to as the brain’s “vomit center,” becomes abnormally stimulated, it can precipitate feelings of nausea and subsequent vomiting.
Furthermore, the trigeminal nerve, which mediates facial sensations, may also undergo abnormal activation. This can trigger the release of neurochemicals that the brain interprets as pain.
One significant neurochemical involved is calcitonin gene-related peptide (CGRP), a protein. Certain injectable migraine therapeutics function by antagonizing this protein to mitigate pain.
Stage 4: Postdrome
The fourth and final phase is known as the “postdrome,” frequently described as the “migraine hangover.”
During this recovery period, the brain actively works to revert to its baseline functionality. This restorative process can result in prolonged fatigue or difficulties with cognitive tasks following a migraine episode.
Strategies for Managing Migraine Attacks
A comprehensive understanding of migraine symptoms and their developmental phases is paramount for effective management.
For individuals experiencing predictable prodromal symptoms, it is advisable to have pain relief medication or anti-nausea tablets readily accessible. This facilitates prompt treatment of emerging symptoms. Recognizing these early signs may also indicate the need for rest, ideally before the headache phase escalates.
During the aura phase, administering migraine-specific analgesics such as triptans, aspirin, or anti-inflammatory agents may prevent the subsequent headache phase from manifesting.
For those experiencing more than four migraine attacks monthly, prophylactic treatments, typically daily oral medications designed to reduce the frequency and intensity of headaches, may be considered. Injectable preventative options are also available.
It is crucial not to disregard the postdrome phase. Exerting oneself excessively during this recovery period can inadvertently trigger overlapping migraine attacks, a scenario where a new episode commences before the preceding one has fully subsided. Such overlapping attacks are significantly more challenging to manage.
Additionally, individuals may experience other accompanying symptoms related to the migraine event, which could include vertigo, cervical discomfort, or tinnitus. Any such ancillary symptoms warrant consultation with a neurologist to rule out more serious underlying pathologies.
Women who experience migraines with aura should consult their healthcare provider prior to initiating hormone-based contraception, as their treatment requirements may differ from those who do not experience aura symptoms.
By thoroughly comprehending the various phases and manifestations of migraine, individuals can be better prepared to confront and manage future attacks.
![]()






