A significant scientific breakthrough has revealed the potential for semaglutide to ameliorate the degenerative tissue damage associated with osteoarthritis, the predominant form of arthritis worldwide.
This pharmaceutical agent, widely recognized for its efficacy in managing type 2 diabetes and promoting weight reduction, is the active ingredient in medications such as Ozempic and Wegovy. However, a recent investigation indicated that semaglutide appears to safeguard joints in murine models via a mechanism distinct from mitigating joint pressure through weight loss.
Rather, the compound appears to reconfigure the metabolic processes within cells responsible for synthesizing and preserving the integrity of healthy cartilage, thereby enhancing their energy production capabilities.
“This research not only underscores the potential extragenic benefit of semaglutide as a potent therapeutic for metabolic osteoarthritis,” state the consortium of researchers from China and the United States in their peer-reviewed publication, “but also elucidates a reparative pathway that is independent of weight reduction.”
Beyond the experimental observations in mice, the research team also conducted a randomized human clinical trial designed to evaluate the impact of semaglutide on the pain levels, functional mobility, and tissue degradation in individuals diagnosed with both osteoarthritis and obesity.
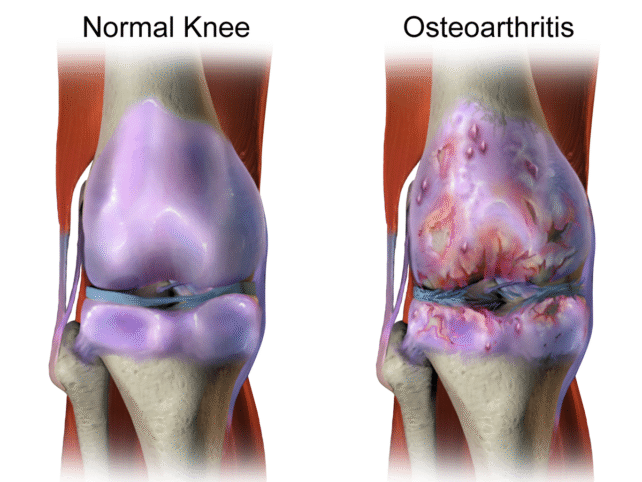
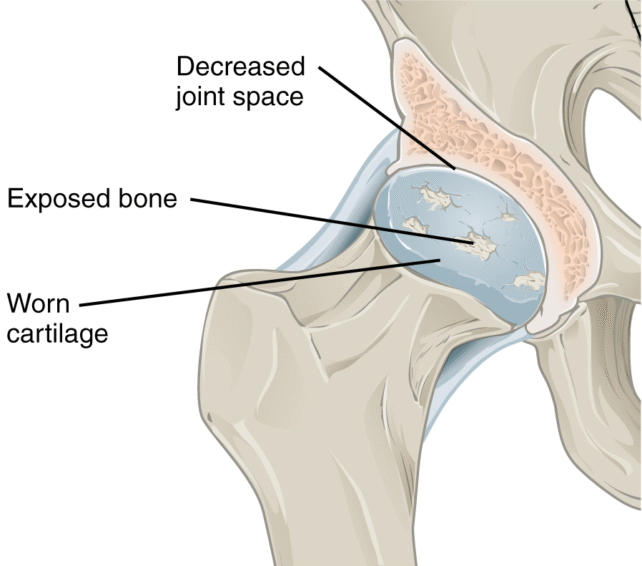
Key factors contributing to the advancement of osteoarthritis include obesity, metabolic derangements such as diabetes, and inflammatory processes. These systemic conditions can exert detrimental effects on virtually all bodily tissues, encompassing bone, cartilage, and the synovium, the specialized membrane lining the internal surfaces of articulating joints.
Medications derived from semaglutide, including Ozempic and similar formulations, function by emulating the action of glucagon-like peptide 1 (GLP-1), a naturally occurring hormone that stimulates insulin secretion to regulate glycemic control. This hormone also signals satiety to the brain, thereby contributing to appetite suppression.
Consequently, it is often presumed that weight reduction alleviates osteoarthritis by diminishing the biomechanical stresses placed upon the joints. However, this correlation is not universally applicable. Conventional therapeutic strategies for osteoarthritis are predominantly symptomatic, offering relief from discomfort but failing to address the underlying pathology.
Conversely, semaglutide appears to exert a beneficial influence on joint health at a foundational biological level. In both rodent models and human subjects afflicted with obesity and osteoarthritis, semaglutide treatment resulted in a reduction in pain perception and a decrease in the rate of cartilage deterioration. Furthermore, the murine subjects exhibited a reduction in osteophyte formation and less severe lesions within their synovial membranes.
Upon comparative analysis of cartilage tissue obtained from treated and untreated mice, researchers identified alterations in the expression profiles of approximately 8,300 proteins.
A critical control mechanism was implemented: a cohort subjected to “pair-feeding,” consuming the same dietary quantity as the semaglutide-administered mice. Despite exhibiting comparable degrees of weight change, this pair-fed group did not experience the same degree of cartilage preservation, strongly suggesting a therapeutic effect on the joint itself that is independent of weight loss.
However, the paramount biological pathway modulated by semaglutide appears to be the “GLP-1R-AMPK-PFKFB3 axis,” a signaling cascade that influences cellular energy metabolism.
By activating this sequence of enzymatic reactions, semaglutide modifies the metabolic pathways utilized by chondrocytes, the cellular components of healthy cartilage, thereby enhancing their metabolic efficiency and promoting cellular survival.
As elucidated by the investigators, the primary energy-generating process for chondrocytes in mice with osteoarthritis was glycolysis.
Glycolysis, an anaerobic metabolic pathway, rapidly provides energy during periods of physiological stress or high-intensity physical activity, such as a rapid morning dash. However, owing to the absence of oxygen, glycolysis yields a limited production of two net adenosine triphosphate (ATP) molecules, the primary energy currency, per molecule of glucose utilized.
To ascertain the potential translational relevance for human subjects, the research team recruited 20 participants, aged between 50 and 75 years, who presented with both obesity and osteoarthritis. These individuals were randomly allocated into two distinct cohorts. One group received sodium hyaluronate (HA), a joint-lubricating agent and a highly bioavailable form of hyaluronic acid. The second group was administered a combination of HA and semaglutide.
Following a 24-week intervention period, the cohort receiving HA in conjunction with semaglutide demonstrated a statistically significant reduction in osteoarthritis-related pain scores and notable enhancements in knee joint functionality. Magnetic resonance imaging (MRI) analyses further revealed an augmentation in cartilage thickness and evidence of recent cartilage regeneration within the medial compartments of the knee, regions critical for weight bearing and shock absorption during everyday activities.
The implications of these research findings could profoundly influence global health outcomes. Osteoarthritis currently affects an estimated 600 million individuals worldwide, with projections indicating that this figure could escalate to one billion by the year 2050. An increasing prevalence is also being observed among younger, physically active demographics, leading to prolonged periods of pain and disability.
This study contributes to an expanding body of evidence suggesting that GLP-1 receptor agonists may confer benefits beyond weight management, thereby refining the pursuit of novel osteoarthritis therapies focused on intracellular metabolic regulation within the joint.
It is, however, prudent to maintain measured expectations. Extrapolating findings from animal models to long-term human outcomes is not always definitive, and the utilization of semaglutide carries its own set of potential adverse effects and considerations.
“The observed protective effects of semaglutide on the human knee joint necessitate a degree of caution in their interpretation and underscore the requirement for further corroboration through additional clinical investigations,” the researchers conclude in their report.
This scientific inquiry has been disseminated in the esteemed journal Cell Metabolism.