The nutrient widely referred to as the “sunshine vitamin” might possess a detrimental aspect. Just as a deficiency in vitamin D can precipitate health hazards, an overabundance carries its own set of risks.
For a considerable duration, medical professionals and researchers have cautioned that vitamin D supplementation is not universally necessary, and in infrequent instances, high-potency formulations can prove deleterious, particularly for pediatric and geriatric populations.
With the escalating prevalence of this supplement, it is now more critical than ever for both patients and healthcare providers to be cognizant of the dosage and the potential adverse effects. While the occurrences of harm are uncommon, they are demonstrably increasing, and in the most severe circumstances, they can be life-threatening.
An excessive intake of vitamin D enhances calcium absorption, potentially leading to hypercalcemia. This condition involves the accumulation of harmful calcium deposits within arteries or soft tissues, thereby escalating the likelihood of kidney stones, disrupting bone metabolism, and inducing a spectrum of distressing symptoms, including but not limited to nausea, emesis, constipation, profound fatigue, muscular weakness, or skeletal discomfort.
The overwhelming majority of individuals recuperate from vitamin D toxicity once the supplementation is halted and they receive supportive care, such as intravenous fluids or pharmacotherapy aimed at reducing calcium levels. However, in exceptional situations, if left unaddressed, vitamin D intoxication can culminate in renal failure necessitating hemodialysis, or tragically, result in fatal gastrointestinal hemorrhage.
Certain research findings even suggest that elderly individuals with elevated serum vitamin D levels might face a higher propensity for accidental falls.
In a comprehensive review conducted in 2018, American researchers highlighted a state of “significant complacency” concerning the potential for vitamin D to exert toxic influences. Definitive consensus among scientists regarding the precise threshold for excessive vitamin D intake remains elusive.
“Concurrently with the pronounced surge in interest surrounding vitamin D, partly propelled by popular literature advocating for high-dose regimens, it is perhaps unsurprising that there has been a notable escalation in reported cases of vitamin D toxicity,” the authors of the 2018 review articulated.
Vitamin D earns its moniker as the sunshine vitamin due to its endogenous synthesis within the body upon exposure to solar radiation. Typically, this photobiological pathway accounts for approximately 90 percent of an individual’s vitamin D requirements, with the remainder being derived from dietary sources, such as oily fish or fortified dairy products.
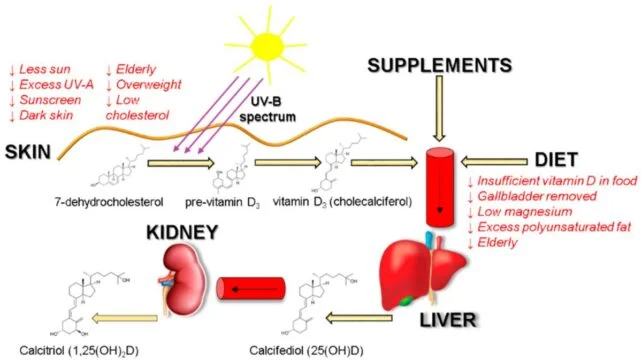
Vitamin D plays a pivotal role in facilitating calcium absorption and supporting essential physiological functions, including immune system regulation, cellular proliferation, metabolic processes, and neuromuscular coordination. A prolonged deficiency in vitamin D can elevate the risk of developing neurological disorders, autoimmune conditions, skeletal pathologies, and cardiovascular ailments.
However, the efficacy of vitamin D supplementation remains a subject of ongoing debate. While certain investigations propose that these supplements may contribute to mitigating the aging process, enhancing cognitive function, or alleviating symptoms of depression, other scientific perspectives have questioned their purported benefits.
Furthermore, these supplementary agents are not devoid of potential hazards. Frequently, instances of vitamin D toxicity arise from errors in the management of vitamin D deficiency.
A notable case illustration involving an octogenarian male revealed that the patient was inadvertently ingesting a high-dose weekly vitamin D tablet, prescribed by his naturopathic physician, on a daily basis. Fortunately, his hypercalcemic state resolved once the error was identified and the supplement was discontinued.
Nevertheless, it is not solely the elderly demographic that requires vigilance regarding their vitamin D intake. In 2016, Denmark’s national health regulatory body mandated a recall for a supplement containing 75 times the recommended vitamin D dosage. Consequently, approximately twenty children experienced adverse toxicological effects from these capsules.
This issue is increasingly prevalent within the United States as well.
Between the years 2000 and 2014, over 25,000 cases of vitamin D toxicity were documented in the US. From 2005 to 2011, these reported incidents saw a staggering increase of 1600 percent, with a significant proportion involving minors and adolescents.
Fortuitously, no fatalities were recorded during this period; however, five cases resulted in severe medical complications.
“Monitor your levels vigilantly,” advises a recent publication on vitamin D from Harvard Medical School, corroborated by journalist and practicing physician Mallika Marshall.
“If you are currently taking a vitamin D supplement, your daily intake likely should not exceed 15 mcg to 20 mcg (600 IU to 800 IU). Unless specifically advised by your medical team, refrain from exceeding 100 mcg (4,000 IU) per day, which is recognized as the established safe upper limit.”
Physicians affiliated with Harvard suggest that individuals diagnosed with a vitamin D deficiency initially focus on consuming foods fortified with this nutrient, as these sources are considerably less likely to induce toxicity.
As is standard medical practice, consulting with a healthcare professional is paramount prior to commencing or discontinuing any form of medication or dietary supplement.