While life-saving chemotherapy and radiation therapies have benefited countless children globally, these intensive treatments carry a significant consequence: a heightened susceptibility to infertility in later adulthood.
Estimates indicate that approximately one-third of males undergoing gonadotoxic interventions, such as chemotherapy or radiation during their formative years, are diagnosed with ‘azoospermia‘ post-puberty. This condition signifies the absence of viable sperm in their ejaculate.
Remarkably, a medical consortium from the University Hospital Brussels and the Free University of Brussels (VUB) has announced a world-first achievement: the reported restoration of sperm production in a patient previously affected by such circumstances.
In a preliminary case report, disseminated prior to formal peer evaluation, the medical team details their innovative approach. They successfully treated a male patient who was azoospermic by reimplanting a segment of his own pre-pubertal testicular tissue into his adult testicle.
The identity of the patient remains confidential. He was initially diagnosed with sickle cell anemia, a hereditary blood disorder managed through bone marrow transplants and limited chemotherapy regimens, bearing resemblance to treatments for certain forms of leukemia.
In 2008, preceding his treatment, the patient, around ten years of age, along with his family, provided consent for the surgical removal of one testicle, with the foresight of cryopreserving it for potential future use.
The individual revisited Brussels IVF at VUB in 2022, expressing a desire to father a child. Diagnostic assessments revealed the absence of viable sperm in his remaining testicle. He subsequently requested the transplantation of the testicular tissue that had been preserved since his childhood.
As part of a clinical investigation, the patient underwent a surgical procedure in 2025 to reintroduce four segments of testicular tissue into his testicle and four into his scrotum.
Presently, approximately one year post-operation, a portion of these grafted tissues are demonstrably generating mature and motile sperm.
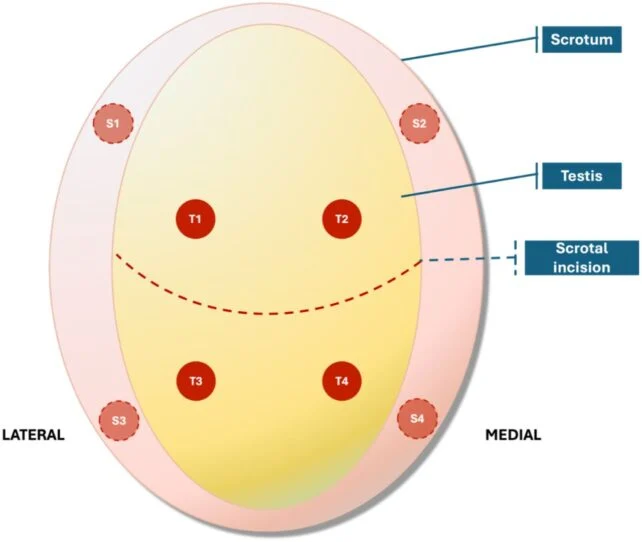
It is important to note that only the sections of the testicle containing the implanted grafts are exhibiting viable sperm, and these are not currently connected to the patient’s vas deferens. Consequently, the sperm are unlikely to be reaching his ejaculate naturally.
Should the patient wish to pursue biological parenthood, it is anticipated that he will require specialized reproductive technologies, such as in vitro fertilization, to combine sperm and eggs.
Nevertheless, the prospect of fatherhood has been established where previously it seemed unattainable.
While this case study awaits rigorous peer review, Dr. Rod Mitchell, a pediatric endocrinologist overseeing a comparable trial at the University of Edinburgh, expressed his long-held expectation that such a procedure would prove successful.
“If tissue is preserved and cells remain viable, their inherent potential should be retained,” Dr. Mitchell conveyed to The Guardian’s Hannah Devlin. “The reintroduction of the tissue into an optimal physiological environment is designed to stimulate it. From a scientific and biological standpoint, the rationale is sound; witnessing it in practice is nonetheless extraordinary.”
For adults undergoing chemotherapy or radiation, conventional sperm banking is the standard recommendation. However, prior to puberty, individuals are not candidates for sperm cryopreservation, as their bodies have yet to achieve the production of mature sperm cells.
Even during childhood, the testicles harbor crucial cells known as spermatogonial stem cells (SSCs), which possess the inherent capacity to develop into sperm later in life. Therefore, preserving this tissue through freezing offers a potential avenue for fertility preservation in at-risk young patients.
The University Hospital Brussels pioneered the practice of freezing immature testicular tissue for the purpose of future fertility preservation in 2002. Since then, numerous other medical institutions have emulated this approach, offering cryopreservation services to over 3,000 boys worldwide, with this number continuing to grow.
These banked samples serve a dual purpose: facilitating ongoing research and providing a resource in the event that future studies validate the efficacy of this method. For a significant number of patients, this represents their sole opportunity for fertility restoration.
Although a single case is insufficient to definitively establish the procedure’s success, the findings from the Brussels case study offer a promising indication that cryopreserved germ cells can withstand the processes of freezing, thawing, and subsequent grafting.
The patient’s cryopreserved, immature testicular tissue exhibited an “exceptionally low number of SSCs.” However, even this minute quantity of cells proved sufficient to initiate sperm generation following reimplantation.
The long-term viability of these grafts beyond one year remains an open question. Existing evidence from animal studies suggests that they may have limited lifespans.
Furthermore, a critical consideration is whether the resulting sperm can successfully lead to the development of healthy offspring.
“This represents a significant advancement in our ongoing scientific endeavor to safeguard the reproductive potential of children diagnosed with cancer or other hematological conditions for their future,” stated fertility specialist Veerle Vloeberghs at Brussels IVF, following the successful transplantation procedure last year. “While the intervention is specifically designed to restore fertility, we are currently unable to guarantee its success or the ultimate ability of patients to conceive children. Nonetheless, this therapeutic approach opens up numerous possibilities for these young individuals, providing them with options that were previously unavailable.”
Researchers are committed to closely observing the progress of the patient who received this groundbreaking testicular transplant as he embarks on his journey toward biological fatherhood.
Their monitoring will encompass the development of embryos, the progression of pregnancies, and the long-term health outcomes of any resultant offspring.
The patient’s narrative is poised to be a source of hope for millions.
The comprehensive study is accessible on medRxiv.