It is projected that pancreatic cancer will ascend to become the second-most prevalent cause of cancer-related mortality in the United States by the year 2030. This grim trajectory is partly attributable to the fact that an overwhelming 85% of identified cases have already progressed to advanced stages by the time of diagnosis.
The fundamental issue lies in our current limitations regarding early disease detection.
However, a novel artificial intelligence model developed collaboratively by researchers from the Mayo Clinic and the University of Texas MD Anderson Cancer Center may herald a significant shift in this paradigm.
This innovative system, designated as REDMOD (radiomics-based early detection model), underwent rigorous evaluation utilizing CT scans from individuals subsequently diagnosed with pancreatic malignancy.
In a remarkable nearly three-quarters of instances, REDMOD successfully identified the most common subtype of pancreatic cancer approximately 16 months prior to its formal diagnosis. This capability nearly doubles the detection efficacy compared to human specialists who reviewed the same scans without the AI’s assistance.
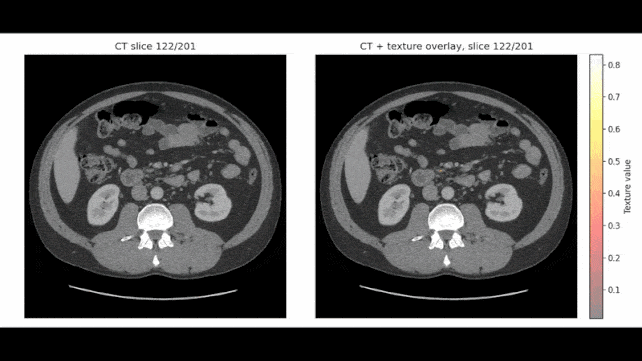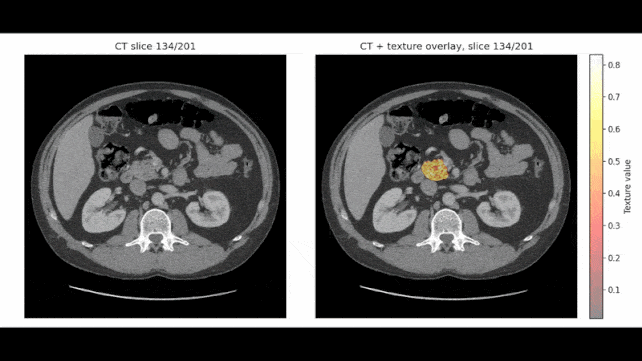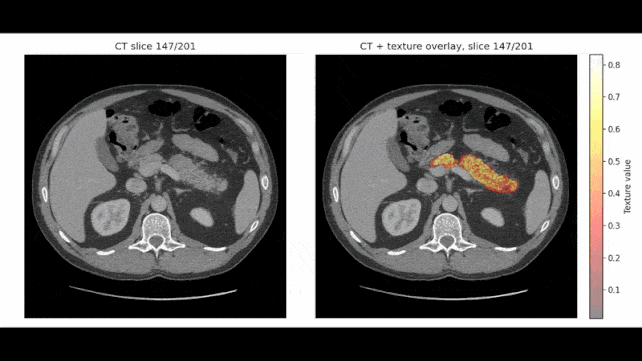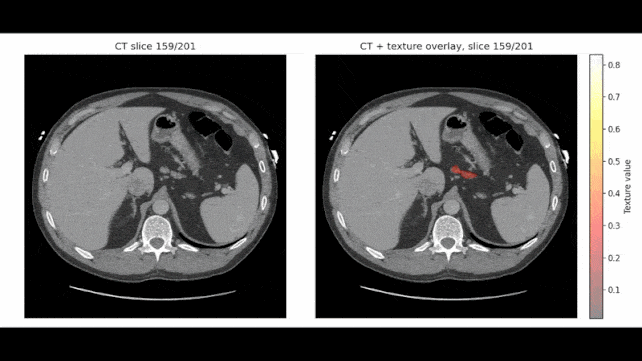
In certain examinations, REDMOD pinpointed aberrant tissue formations over two years before a diagnosis was established, with the research team expressing confidence in its potential to detect the malignancy up to three years in advance.
“Our greatest impediment to mitigating fatalities from pancreatic cancer has historically been our inability to identify the disease in its nascent, treatable stages,” stated Ajit Goenka, a radiologist and nuclear medicine specialist affiliated with the Mayo Clinic.
“This artificial intelligence is now capable of discerning the distinct markers of cancer within a pancreas that appears normal, and it can perform this reliably across varied temporal intervals and diverse clinical environments.”
To facilitate REDMOD’s learning process and its capacity to identify the subtle hallmarks of cancer in its nascent phases, researchers employed a dataset comprising 969 pancreatic CT scans for its training.
Rather than focusing on the presence of an overt tumor, the model is engineered to detect radiomic signatures, which represent subtle alterations in tissue texture and structural integrity often imperceptible to the unaided human eye.
Many malignant growths originate from normal cells undergoing DNA mutations that impact their proliferative and division processes. However, it can require years for these genetic changes to manifest as a tumor substantial enough to elicit symptoms or become clearly discernible on imaging.
Following the initial instructional phase, REDMOD was subjected to scrutiny using a distinct cohort of CT scans: 63 from individuals who were eventually diagnosed with cancer but whose scans were acquired prior to their diagnosis, and 430 from healthy individuals who did not have the disease.
From the group of 63 individuals diagnosed with cancer, REDMOD correctly identified 46 as exhibiting suspicious characteristics, achieving a classification accuracy rate of 73 percent (equating to almost three out of every four cases).
It is noteworthy that all these scans had previously been deemed free of malignancy by human radiologists. In a concurrent review, two radiologists examining the scans alongside REDMOD were only able to identify early indicators of cancer in 38.9 percent of these instances.
Regarding the 430 healthy control subjects, REDMOD erroneously flagged 81 as suspicious. Consequently, had this AI system been implemented in a real-world clinical setting, these individuals might have been summoned for supplementary investigations before ultimately being cleared.
A comparable level of performance was observed across two additional dataset evaluations, which involved utilizing different imaging equipment at distinct medical facilities.
Furthermore, for patients with multiple available scans, the AI system consistently produced largely congruent results, even when those scans were acquired at different points in time, separated by several months.
“These aforementioned capabilities position the model for prospective validation within high-risk populations, a crucial prerequisite for transitioning the diagnostic paradigm from late-stage symptomatic identification to proactive pre-clinical intervention,” articulate the study’s authors in their published findings.
The underlying rationale is that the earlier REDMOD gains access to CT scans—potentially those administered routinely for other medical conditions or purposes—the greater its potential utility will be. It is conceivable that this technology could identify pancreatic cancer at a stage where curative therapeutic interventions remain a viable option.
Nevertheless, further development is imperative before this objective can be realized. The immediate next steps for the researchers involve assessing the AI’s performance across larger, more heterogeneous patient cohorts and evaluating the ease with which clinicians can integrate it into their established diagnostic workflows.
The research team expresses considerable optimism regarding these initial outcomes, harboring the hope that with continued refinement and optimization, this AI system could evolve into an exceptionally valuable tool for combating one of the most lethal forms of cancer.
“The demonstrated capacity of this framework to consistently detect these subtle, hidden signals within a substantial dataset of clinical relevance, complemented by its high longitudinal consistency and validated specificity, establishes a robust foundation for AI-enhanced early detection,” conclude the researchers.