A recent comprehensive analysis of extant research findings has established a significant correlation between cannabis use disorder and major depressive disorder.
The precise etiology of this observed association remains elusive.
It is yet to be determined whether problematic cannabis consumption precipitates depressive symptoms, or if individuals experiencing depression resort to cannabis as a form of self-medication.
Furthermore, there is a possibility that shared underlying risk factors contribute to the manifestation of both conditions. Although the co-occurrence of these two disorders is recognized, a more extensive body of data is requisite to fully elucidate their intricate relationship.
An international consortium of investigators undertook a global examination of the available evidence, particularly in light of the evolving legal status of cannabis in various jurisdictions worldwide.
This extensive review encompassed 55 prior investigations, involving a participant pool exceeding 3.2 million individuals, including close to half a million diagnosed with cannabis use disorder (CUD). Additionally, over 100,000 participants were identified as having major depressive disorder (MDD).
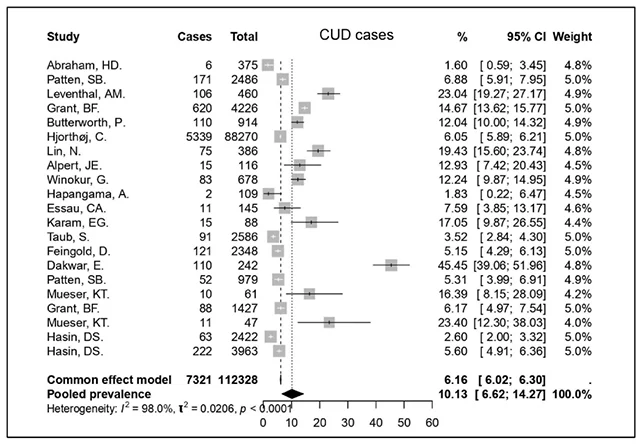
The researchers assessed the incidence of MDD within the CUD cohort and, conversely, the prevalence of CUD among those with MDD. Their findings indicated that depression appears to augment the probability of cannabis utilization, while cannabis use seems to elevate the risk of developing depression.
It is noteworthy that in certain US states, medical cannabis is occasionally prescribed for the management of MDD.
The investigation revealed that approximately 32 percent of individuals afflicted with CUD also presented with MDD. Concurrently, CUD was reported by slightly more than 10 percent of those diagnosed with MDD.
These figures represent a considerably higher prevalence than that observed for either condition within the general populace.
Within a segregated analysis, the research team discerned that the two conditions exhibit a connection even when they do not manifest concurrently.
“Collectively, these discoveries suggest that MDD is a prevalent comorbidity across all demographic segments of individuals diagnosed with CUD, with notably elevated rates observed in psychiatric settings and when employing lifetime diagnostic criteria,” the research team stated.
“Discrepancies between psychiatric and community-based cohorts – particularly the markedly higher current CUD prevalence among patients diagnosed with MDD – underscore the imperative for systematic screening protocols across all treatment modalities.”
It is important to emphasize that these findings do not establish causality, as the review was not designed to ascertain cause-and-effect relationships. Instead, it involved the aggregation of existing studies rather than the longitudinal observation of a single new cohort.
Despite the robust association identified, definitive conclusions regarding whether MDD initiates CUD, or vice versa, cannot be drawn. Furthermore, even with further investigation, the interplay between cannabis use and depression may prove challenging to disentangle in practical scenarios. For instance, symptoms associated with cannabis withdrawal, such as anxiety and sleep disturbances, can closely resemble those of depression.
What can be confidently asserted is that this review synthesizes a substantial body of data, providing our most comprehensive understanding to date of the nexus between the excessive use of cannabis and serious, persistent depressive states.
Previously, cannabis has been implicated in alterations of gene expression and an increased susceptibility to cardiovascular disease, while depression is associated with severe illnesses and an elevated risk of dementia.
Cannabis use disorder is characterized by a dysfunctional pattern of cannabis consumption that may involve intense cravings, withdrawal symptoms, escalating tolerance, and an inability to reduce use despite adverse repercussions.
Major depressive disorder is identified by a sustained period of low mood or diminished interest, accompanied by symptoms such as disrupted sleep, profound fatigue, and impaired cognitive function.
The ultimate objective is to leverage a more profound comprehension of the link between these conditions to facilitate their effective management and appropriate therapeutic interventions.
The researchers highlight the clinical significance of this, as in individuals presenting with both disorders, one condition may be inadvertently overlooked or receive diminished attention when the other is undergoing treatment.
“These findings underscore the critical importance of concurrently addressing both conditions within clinical and research frameworks,” the review authors concluded.
“While pharmacotherapeutic strategies for comorbid CUD and MDD remain equivocal, psychological interventions such as cognitive behavioral therapy and motivational interviewing demonstrate considerable promise and merit additional exploration.”