A diagnostic blood examination demonstrates considerable promise for forecasting the nascent phases of Alzheimer’s disease, potentially impacting individuals decades prior to the manifestation of overt symptoms.
Subsequent to investigations spearheaded by a consortium from Mass General Brigham in the United States, it was ascertained that a specific blood biomarker, designated as pTau217, could serve as an antecedent indicator of the potential for deleterious congregations of amyloid-beta and tau proteins within the cerebral cortex.
The accumulation of these specific protein aggregates has been consistently correlated with the etiology of Alzheimer’s disease.
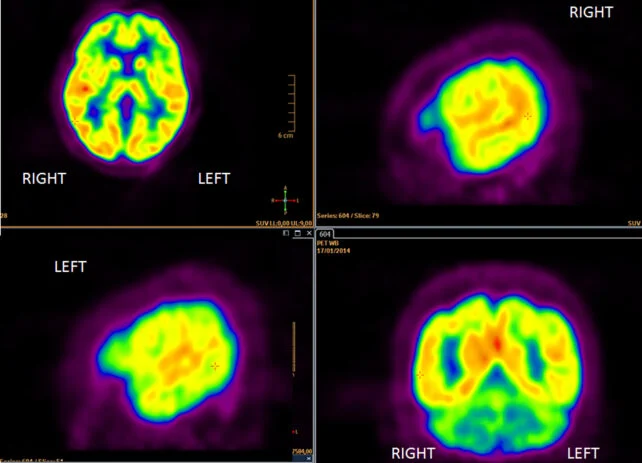
Presently, advanced imaging modalities such as PET (positron emission tomography) brain scans are frequently employed to detect these pathological markers. However, it is conceivable that pTau217 blood analyses could facilitate the identification of individuals at elevated risk for Alzheimer’s disease with unprecedented earliness.
“Previously, our understanding posited that PET scan detection represented the earliest discernible indicator of Alzheimer’s disease progression, revealing amyloid deposition in the brain approximately ten to twenty years before the onset of clinical symptoms,” explains the principal investigator, Hyun-Sik Yang, a neurologist affiliated with Mass General Brigham.
“However, our current findings suggest that pTau217 can be identified many years prior to the development of clearly evident abnormalities apparent on amyloid PET scans.”
The research endeavor involved the recruitment of 317 participants, with age demographics spanning from 50 to 90 years. All enrolled volunteers maintained cognitive health at the commencement of the investigation and were monitored for an average duration of eight years.
Comprehensive data encompassing results from amyloid-beta and tau PET scans, cognitive assessments, and circulating pTau217 levels derived from blood samples were meticulously collected, integrated, and longitudinally analyzed.
The blood analyses were demonstrated to achieve a high degree of concordance with PET scan findings concerning the presence of proteinous tangles and aggregates. In certain instances, escalating pTau217 concentrations served as a predictor of alterations that preceded their detection on cerebral imaging.
Put another way, the investigators observed that elevated pTau217 levels were indicative of a predisposition towards subsequent Alzheimer’s-related pathology, whereas diminished pTau217 concentrations suggested a minimal likelihood of disease manifestation.
“A particularly noteworthy observation from our study is that even when amyloid scans appear unremarkable in a clinical setting, the pTau217 biomarker has the capacity to identify individuals who subsequently test positive for amyloid,” states Yang.
“Furthermore, it indicates that individuals exhibiting low pTau217 levels are likely to remain amyloid-negative for an extended period.”
Elevated concentrations of pTau217 were also associated with an increased probability of cognitive decline throughout the study’s duration, although this correlation was primarily observed in participants presenting with initial indications of toxic amyloid-beta protein accumulation at baseline.
This recent research corroborates prior findings suggesting that circulating pTau217 in the bloodstream could serve as a valuable adjunctive tool for evaluating Alzheimer’s risk. It may function as a sensitive biological indicator of nascent pathological processes within the brain.
Nevertheless, the widespread integration of this methodology into clinical practice is anticipated to require a considerable timeframe. The research team aims to accumulate supplementary data to enhance the precision of prognostic algorithms, necessitating the inclusion of larger and more heterogeneous participant cohorts.
An additional consideration is that even if blood tests can accurately forecast the development of amyloid-beta or tau protein accumulations in the brain, these pathological changes may not invariably progress to the debilitating state of dementia.
Currently, medical practitioners employ a multifaceted array of diagnostic tests and evaluations to confirm an Alzheimer’s diagnosis. A singular, definitive test capable of reliably predicting an individual’s risk years or decades in advance is not yet available.
“Given the dynamic and rapid advancement within this scientific field, we are enthusiastic about observing discoveries originating from research settings being expeditiously translated into practical clinical applications,” comments neurologist Jasmeer Chhatwal, also from Mass General Brigham.
“By proactively identifying individuals who are predisposed to becoming amyloid-positive in the future, we endeavor to preemptively intervene, thereby facilitating earlier detection of Alzheimer’s disease.”